The food chatter just stopped.
That’s how people on semaglutide describe it .Not reduced hunger, not weaker cravings, but a silence where background noise used to be. Researchers weren’t expecting that report. The drug was designed to suppress appetite, not to quiet something that sounds more like a mental frequency. This leads to a question that neuroscience is only just beginning to answer: what was actually making that noise in the first place?
The answer starts with recognizing that food noise and food cravings are not the same thing. They don’t appear to arise from the same brain regions, they don’t follow the same behavioral rules, and they may not respond to the same interventions. The confusion between them is expensive, not just intellectually, but practically, in how people try to manage their relationship with food.
A note on language first: “food noise” is a patient-reported and clinical observation term that gained traction largely through GLP-1 medication discourse. It hasn’t yet been formally operationalized as a neuroscientific construct with its own dedicated imaging literature. What the brain scan data can offer is a framework for thinking about what kind of phenomenon it might be and why that distinction matters.
Two signals that feel similar but run on different hardware
A craving is directed. It points at something specific , the smell of something cooking, a particular time of day, a familiar stress state. It has a quality of urgency that builds and, if left alone, eventually passes. Cravings are episodic events. They arrive, they peak, they leave.
Food noise is different in character. Think of it less like a wave and more like a browser tab running in the background — persistent, low-grade, not pointing at anything in particular. What’s in the refrigerator. What you’ll eat next. Whether the portion was right. What you could have instead. It doesn’t necessarily have the intensity of a craving. It has duration instead.
Both get filed under “thinking about food too much,” which is why they tend to receive the same advice: resist, distract, have more willpower. That advice is calibrated for one system. The evidence suggests the other system may not respond to it at all .Not because the effort is insufficient, but because the wrong mechanism is being addressed.
It’s also worth noting that these systems interact rather than operate in isolation. The reward network and broader cognitive regulation networks are in constant conversation. Think of this as a way to identify which system is taking the lead, rather than a claim that the brain runs two entirely separate programs. It’s a simplification to make the concept easier to follow.
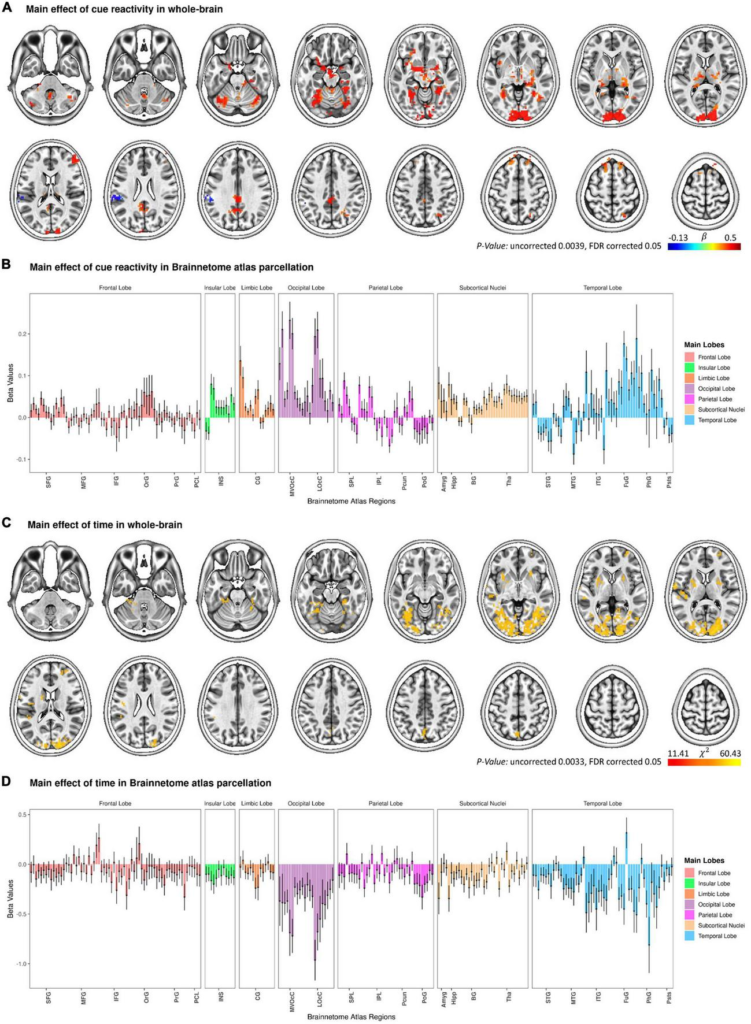
The clearest picture of food cravings in the brain came from a 2004 study by Pelchat and colleagues, who used fMRI to image people actively experiencing them. The activation pattern that emerged was the mesolimbic dopamine system , the brain’s reward anticipation circuit.
The key regions: the nucleus accumbens, the ventral tegmental area (VTA), the insula, and the amygdala. This is the same circuit that activates in response to other kinds of anticipated reward , whether thats money, social connection, and in people with addiction histories, drug-related cues. The brain isn’t experiencing the reward yet. It’s predicting it, and that prediction generates a motivational pull of its own.
The insula’s involvement is particularly specific. This region processes interoceptive signals , what the body is sensing from the inside. A craving isn’t purely cognitive. It has a physical texture: the slight increase in saliva, a tension in the chest, a pull toward movement. These are insula outputs.
Later work on food cue reactivity reinforced the pattern: cravings are largely cue-driven.Over time, the brain maps out associations where specific places, times, feelings, or smells signal a coming reward. When those cues pop up, the dopamine system kicks in before you even take a bite. This is why cravings feel so context-dependent. The signal isn’t originating purely from inside the body. It’s being triggered by learned patterns in the environment.
The practical implication: a craving is the dopamine prediction system operating correctly. It has learned associations, and it’s acting on them. This framing is consistent with the established hedonic and reward network model for obesity, as described in the Handbook of Obesity (Bray & Bouchard, 5th ed.), which identifies the nucleus accumbens, dopamine pathways, and the limbic system as central to hedonic eating and motivational drive.
What may underlie food noise: a loop that won’t close
Food noise does not appear to be primarily a reward anticipation phenomenon. The pattern it most resembles , persistent, involuntary, not driven by hunger or desire, has more in common with ruminative thought than with reward-seeking.
Neuroscience gets a bit more speculative here. The Default Mode Network (DMN) is known as the brain’s baseline system, which stays busy during mind-wandering, self-reflection, and repetitive thought loops (Buckner, Andrews-Hanna & Schacter, 2008). Its main hubs include the posterior cingulate cortex, the medial prefrontal cortex, and the angular gyrus.
What is less established and worth stating directly is the specific role of the DMN in food-related cognition and obesity. The DMN does not appear in the standard obesity neuroscience framework, which centers on the homeostatic regulatory network (hypothalamus, arcuate nucleus, leptin-melanocortin pathway), the hedonic reward network, and the vagal-afferent network. However, emerging 2024 – 2025 research is beginning to show DMN alterations in people with obesity including changes in posterior cingulate and angular gyrus connectivity in patients with abdominal obesity suggesting the network may be relevant to the broader picture, even if the mechanisms aren’t yet mapped.
The more established piece is this: intrusive, repetitive thought patterns in general including food-related preoccupation in eating disorder research are associated with reduced lateral prefrontal cortex engagement. The lateral PFC is a key site of executive control and thought suppression. When its activity is dampened, unwanted thoughts have less resistance to their recurrence. This pattern has been observed in ruminative states more broadly, and the phenomenology of food noise ,persistent despite effort, unconnected to hunger is consistent with it.
The OCD-spectrum comparison that sometimes appears in this discussion deserves a careful qualifier. The phenomenological resemblance is real: intrusive thoughts that recur despite attempts to suppress them, without being driven by reward anticipation. But OCD involves distinct compulsive neutralizing behaviors that are not necessarily present in food noise, and claiming structural equivalence goes further than the current evidence supports. The more accurate framing is that food noise shares some characteristics with ruminative thought loops and may respond to some of the same cognitive regulation approaches without being the same phenomenon.
How GLP-1 medications reach both systems — and what remains unknown
This neurological distinction helps make sense of a pattern clinicians and patients have both noticed: GLP-1 medications like semaglutide appear to address both cravings and food noise, but through mechanisms that feel qualitatively different.
The appetite and craving effects are documented and mechanistically grounded. These medications act on GLP-1 receptors in the hypothalamus and communicate via vagal afferent pathways, the nerve channels running between the gut and the brain. By modulating satiety signaling and reducing the reward salience of food cues, they act on the mesolimbic circuit. Less dopamine prediction error. Less cue reactivity. The craving signal softens. This is consistent with the established GLP-1 mechanism described in the obesity literature, and with a 2025 Cell Metabolism study confirming that semaglutide’s weight-related neural effects are mediated primarily through Adcyap1+ neurons in the dorsal vagal complex and downstream satiety structures , a brainstem and hindbrain pathway.
The food noise reports are a different matter. When users describe “the chatter stopping,” they’re describing something that sounds cognitive rather than appetitive , closer to a mental quieting than a physical one. Whether this reflects any direct effect on ruminative thought networks is genuinely not established. A small number of studies have looked at GLP-1 effects on brain connectivity, with preliminary signals in some cognitive networks, but there is no robust neuroimaging evidence confirming a GLP-1 DMN link in humans.
What can be said more carefully is this: the subjective reports are consistent enough across clinical contexts to be worth taking seriously as a signal, even before the mechanism is mapped. They suggest that whatever is producing food noise is being affected but the pathway from GLP-1 receptor activation to cognitive quieting remains an open question in the literature. That’s not a reason to dismiss the report. It’s a reason to keep investigating it.
What this means for choosing the right tool
The distinction has a practical application, even where the science is partial.
If the primary experience is cravings episodic, cue-triggered, reward-anticipation-driven the interventions that target the dopamine prediction system make logical sense. Cue exposure and response prevention protocols. Blood sugar stabilization to reduce physiological triggers. Attention to the learned associations between particular environments or emotional states and eating behavior. These address the right system.
If the primary experience is food noise persistent, involuntary, loop-like, not connected to actual hunger or desire a different set of tools becomes relevant. Certain mindfulness protocols specifically designed to interrupt ruminative thought patterns (not all mindfulness practice is equivalent here). Sleep, which is one of the strongest regulators of resting-state network coherence. Metabolic stability, which reduces the brain’s ambient stress response and may free up executive resources. Cognitive approaches targeting intrusive thought suppression failures. These are aimed at the loop, not the reward signal.
Treating food noise as though it were a craving trying to resist or redirect something that isn’t directional may be a category error. The effort doesn’t reach the right system. When it doesn’t work, the default conclusion tends to be something about the person’s willpower or discipline, rather than something about the model being applied.
The brain scan data available on food cravings is robust and well-replicated. The picture for food noise is less complete the construct itself is still being translated from patient report into research protocol. But the preliminary direction of the evidence, and the clinical pattern of what helps and what doesn’t, suggests the two phenomena are genuinely different in character.
“The food chatter stopped” turns out to be a precise observation. Something in a loop-closing mechanism shifted. What exactly that mechanism is, and whether it can be reliably influenced not just by medication but by targeted cognitive and metabolic approaches is the question worth following.
Join the Field Notes
Metabolic Field Notes tracks the evidence as it develops, without protocol-pushing and without hype. If evidence-aware, translational science is useful to you, join the Field Notes.
Medical Disclaimer: The content on this blog is for informational and educational purposes only and does not constitute professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.


